Why Hyperbaric Oxygen Can Treat Hand Injuries
2025-12-04Editor's Note:
Hyperbaric oxygen therapy increases blood oxygen partial pressure and tissue oxygen supply, rapidly improving local ischemia and hypoxia after hand injuries. It inhibits anaerobic bacterial growth to prevent infection, promotes angiogenesis and granulation tissue formation, and accelerates wound healing. Additionally, it reduces edema and inflammation, alleviates nerve compression due to post-injury swelling, aids nerve function recovery, and lowers the risk of tendon adhesions and tissue necrosis.

Hand injuries are among the most common clinical traumas. Given the critical importance of hand function, accurate diagnosis and primary repair of damaged tissues are essential steps in restoring hand functionality. Hyperbaric oxygen therapy serves as an effective treatment for hand injuries and is a key component of comprehensive management.
Key Diagnostic Points
Obtain a detailed history of the injury, including the mechanism, nature, timing, and circumstances.
Examine the hand wound:
Determine the location, size, type of injury, and extent of skin loss to plan wound closure.
Assess deep tissue involvement (nerves, tendons, bones, and joints). X-rays should be taken if necessary.
Evaluate vascular injury:
Check finger color, temperature, pulse, and capillary refill (blanching test).
Use the Allen test to assess the integrity of the ulnar and radial arteries, as well as the superficial and deep palmar arches, to guide treatment decisions.
Assess nerve damage:
Examine the ulnar, median, and radial nerves for potential injury.
Evaluate tendon injuries:
Observe changes in the resting posture of the hand and assess active finger flexion and extension to identify tendon damage.
Check for bone and joint injuries:
Look for localized pain, swelling, shortening, angulation, rotational deformities, or abnormal movement. Confirm with X-rays.
Conduct a systemic assessment to identify any associated injuries and provide appropriate treatment.
Surgical Management
Principles of Hand Injury Management:
Emergency Care: Focus on hemostasis, reducing contamination, preventing further injury, and ensuring prompt transport. Local pressure dressing is the simplest and most effective method for bleeding control. Tourniquets should only be used if compression fails, with careful timing (release for 5 minutes every hour).
Early and Thorough Debridement: Perform within 6–8 hours. Remove all necrotic, non-viable tissues and foreign bodies. Preserve finger length whenever possible.
Management of Deep Tissue Injuries: Aim to repair damaged bones, joints, tendons, vessels, and nerves primarily during debridement. In cases of severe contamination or injuries beyond 12 hours, reduce and stabilize fractures/dislocations. Delayed repair of tendons and nerves may be performed after wound healing.
Early Wound Closure: Use primary suturing, "Z"-plasty for wounds crossing joints, parallel to web spaces, or perpendicular to skin lines to prevent scar contracture. For skin defects, opt for split-thickness skin grafts or flap coverage. Free vascularized flaps may be considered for one-stage closure.
Postoperative Care: Immobilize the hand in the functional position with fingers separated and bandaged. Leave the radial pulse accessible for monitoring. Elevate the limb to reduce swelling. Initiate early mobilization and functional exercises after removing external fixation.
Management of Hand Fractures and Dislocations:
Achieve accurate reduction and stabilization early, using methods that allow early functional exercise.
Close wounds promptly to minimize infection and granulation tissue formation, reducing scar-related dysfunction.
Avoid immobilizing uninjured fingers. Generally, dislocations are fixed for 3 weeks, fractures for 4–6 weeks. Begin functional training promptly after removal.
Tendon Injury Management:
Strive for primary repair of all damaged tendons.
Employ microsurgical techniques using 7-0 or 8-0 sutures for optimal outcomes.
Encourage early active extension and protected passive flexion postoperatively.
Nerve Repair:
Primary microsurgical repair is recommended for all severed hand nerves. If conditions are unfavorable (e.g., severe contamination, >12 hours post-injury), perform delayed repair after wound healing.
Timely and appropriate functional exercise is crucial for restoring hand function.
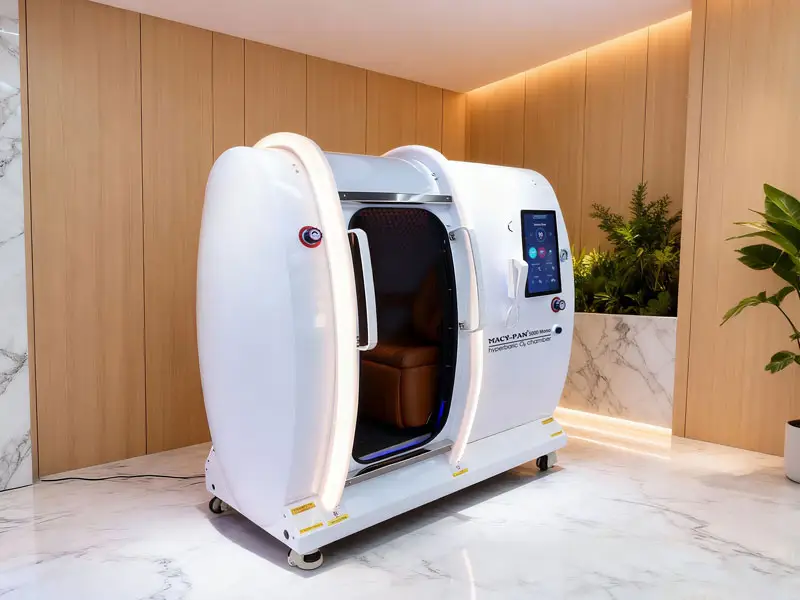
Hyperbaric Oxygen Therapy (HBOT)
Mechanisms of Action:
- Improves oxygen delivery to injured tissues, protects damaged cells, reduces inflammation, and minimizes necrosis.
- Enhances vascular permeability, alleviates edema and swelling, and improves local circulation.
- Stimulates tissue regeneration and accelerates wound healing.
- Promotes the establishment of collateral circulation.
Indications:
- Severe hand crush or avulsion injuries.
- Impaired local circulation following hand trauma.
- Post-surgical repair of fingertip amputations.
- Post-neural anastomosis.
Protocol:
- Pressure: 1.6–2.2 ATA
- Duration: 60–90 minutes per session
- Frequency: 1–2 sessions daily
- Total Course: 20–30 sessions
Efficacy:
HBOT for hand injuries rapidly reduces local swelling, improves circulation, minimizes tissue necrosis, accelerates wound healing, and significantly lowers the risk of long-term complications.
Source of the Article:Zaozhuang Hyperbaric Oxygen
Hey, I’m Macy-Pan
1# Hyperbaric Oxygen Chamber Manufacturer in China. 18 years of industry experience. 126 countries and regions reached