A Non-Drug Support for Sleep Disorders—HBOT
2026-02-28Article forwarded from Ma Jindong, Health Oxygen Therapy
Governed by the central nervous system, sleep is the body's symphony of restoration, guiding the mind and body into a unified state of recovery and repose. This biological imperative is critical for survival, with its significance manifesting across multiple key dimensions: it not only promotes tissue repair and enhances immunity but also helps the brain consolidate memories, regulate emotions, maintain endocrine and metabolic balance, and support daytime cognitive functions and social abilities. Long-term lack of quality sleep significantly increases the risk of various conditions such as anxiety, depression, hypertension, and diabetes.
Statistics show that approximately one-third of the global population experiences sleep disorders to varying degrees. In China, 48.5% of adults report sleep-related issues (source: 2025 China Sleep Health Survey Report). Sleep problems have become a significant public health concern worldwide.
Current treatment options for sleep disorders are diverse, primarily divided into non-pharmacological and pharmacological approaches. Non-pharmacological treatments include cognitive-behavioral therapy, sleep hygiene guidance, psychological counseling, acupuncture, and physical therapies. Pharmacological treatments involve the use of sedative-hypnotics or anti-anxiety/depression medications under medical supervision. Among these, hyperbaric oxygen therapy (HBOT), a traditional physical treatment, has gained increasing attention in recent years as an adjunctive therapy for sleep disorders. This article systematically explores the connection between HBOT and sleep disorders, discussing its mechanisms, applicable scenarios, limitations, and clinical recommendations.

1. Common Types and Causes of Sleep Disorders
Sleep disorders refer to a range of conditions characterized by abnormal sleep duration or quality that impair daytime functioning. They are mainly categorized into five types:
Insomnia
Circadian rhythm sleep disorders
Sleep-related breathing disorders
Parasomnias
Sleep-related movement disorders
The causes of sleep disorders vary across types but share common underlying factors, including social environment, psychological stress, medical conditions, and medications. Chronic cerebral hypoxia, neurotransmitter imbalances, and systemic inflammation are common pathological bases for many sleep disorders.

2. How Hyperbaric Oxygen Improves Sleep Disorders
HBOT does not work by directly inducing sedation but by repairing physiological mechanisms related to sleep regulation. Its core mechanisms include:
(1) Correcting Cerebral Hypoxia and Repairing Neurons
The brain has a high demand for oxygen. Chronic insomnia often leads to mild hypoxia and micro-inflammation in key sleep-regulating areas such as the prefrontal cortex and thalamus. HBOT significantly increases blood oxygen levels, allowing large amounts of oxygen to dissolve directly into the plasma and reach hypoxic brain tissues. This corrects cerebral hypoxia and supports mitochondrial aerobic metabolism, increasing ATP production to repair neurons damaged by oxygen deficiency. For patients with sleep apnea syndrome, HBOT also directly alleviates nighttime hypoxia, reducing awakenings and improving sleep continuity.
(2) Regulating Neurotransmitters and Creating an Optimal Brain Environment
Neurotransmitters play a key role in sleep regulation. HBOT helps improve sleep by modulating the synthesis and metabolism of neurotransmitters such as serotonin and GABA, while enhancing melatonin secretion to stabilize the sleep-wake cycle. Additionally, HBOT suppresses brain inflammation by reducing pro-inflammatory factors like TNF-α and IL-6, which interfere with sleep, thus creating a favorable cerebral environment for rest.
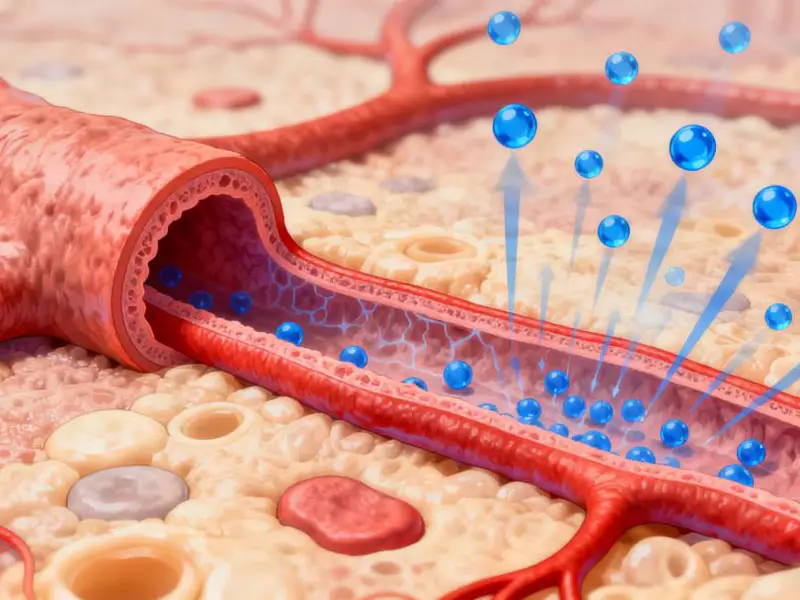
(3) Improving Vascular Function and Reducing Tissue Edema
HBOT promotes moderate vasoconstriction, reducing vascular permeability and minimizing tissue fluid leakage and edema. This expands the effective diffusion distance of oxygen, ensuring that even tissues far from capillaries receive adequate oxygen. Improved microcirculation also aids in the removal of metabolic waste, alleviating discomfort caused by ischemia and hypoxia, and helping the body relax into a state conducive to sleep.
(4) Alleviating Anxiety and Aiding Psychogenic Insomnia
Some sleep disorders are closely linked to anxiety. While addressing tissue hypoxia, HBOT can modulate autonomic nervous function to reduce anxiety. Clinical cases have shown that patients experiencing anxiety-induced insomnia due to unfamiliar hospital environments or health concerns often see significant sleep improvements after several HBOT sessions, along with enhanced daytime alertness.
3. Suitable Candidates for HBOT in Sleep Disorders
HBOT is not a universal “insomnia cure” but is particularly beneficial for sleep disorder patients with clear hypoxia or neurological damage. Suitable candidates include:
Patients with sleep apnea syndrome (especially those with AHI >15 events/hour accompanied by daytime sleepiness and memory decline).
Patients with sleep disorders following traumatic brain injury or stroke.
Individuals with refractory insomnia who experience poor results with sleep medications or are concerned about side effects.
Brain workers and elderly individuals with chronic fatigue syndrome accompanied by insomnia.
Patients with anxiety or depression combined with sleep disorders and signs of cerebral hypoxia.
4. Recommendations for Using HBOT in Sleep Disorders
For those considering HBOT, it is essential to follow the principles of scientific assessment, standardized treatment, and combined interventions:
(1) Accurate Assessment and Clear Diagnosis
Given the complex causes of sleep disorders, it is recommended to undergo tests such as polysomnography to determine the type of insomnia and whether hypoxia is present. A joint evaluation by hyperbaric oxygen specialists and relevant medical departments should determine suitability for HBOT. For non-hypoxia-related insomnia, priority should be given to psychological or pharmacological treatments.
(2) Standardized Treatment and Controlled Sessions
HBOT must follow individualized protocols, including treatment pressure, frequency, and duration, adjusted by a doctor based on the patient’s condition. Over-treatment should be avoided to minimize side effects.
(3) Combined Interventions for Enhanced Efficacy
HBOT works best when combined with good sleep habits. During treatment, maintain regular sleep schedules, avoid electronic devices before bedtime, keep the bedroom at a comfortable temperature and humidity, and reduce caffeine and alcohol intake. For insomnia rooted in psychological factors, combining HBOT with cognitive-behavioral therapy is recommended.
5. Conclusion
Hyperbaric oxygen therapy offers a safe, non-drug adjunctive treatment option for specific types of sleep disorders, particularly those related to hypoxia or neurological damage. Its core value lies in correcting cerebral hypoxia and restoring neurotransmitter balance to repair sleep regulation mechanisms. However, it is crucial to identify appropriate candidates and avoid replacing conventional treatments or overusing HBOT. For individuals with sleep disorders, a professional evaluation to determine the underlying cause is recommended. Under medical guidance, an individualized treatment plan combining HBOT with sleep hygiene and psychological interventions can more effectively improve sleep quality.
Hey, I’m Macy-Pan
1# Hyperbaric Oxygen Chamber Manufacturer in China. 18 years of industry experience. 126 countries and regions reached